Dr. Elliott’s Personal Journey with Neuralgia
Even if you’ve heard about Trigeminal Neuralgia, you may not know that over a third of patients who have it admit to having suicidal thoughts because of the severity of the pain, and at least 50% of them develop clinical depression.
I learned about trigeminal neuralgia in medical school and residency but until I suddenly experienced it in 2020, I couldn’t relate to the degree of pain it causes.
In 2020, while I was standing in an exam room at work, I felt a sudden bolt of what I can only describe as the sensation of a downed power line suddenly contacting the area between my right eye and scalp. I felt like that part of my face was being electrocuted. The pain was so intense that it made me freeze for 2 minutes, unable to talk, open my eyes, or even move. My medical assistant was with me when it happened and she almost called 911 when she saw me totally freeze for so long.
I knew immediately that I was experiencing supraorbital trigeminal neuralgia.
Over the following month, I had multiple episodes a day lasting from less than a second to up to two minutes at a time, sometimes only several minutes apart. The pains occurred spontaneously but definitely when I touched the skin between my right eye and scalp. I was unable to apply makeup to the right upper side of my face, wash or even gently comb my hair in that area, and if a strong breeze blew on my face, I was guaranteed to experience a full 2 minutes of severe electrical shock-like pain.
I understood then why people with trigeminal neuralgia consider suicide. I doubt I’d still be alive if I hadn’t found a way to at least partially control the pains.
I learned to start counting the seconds when the pain hit because I knew that by the end of the second minute, the nerve would wear out for a while, but the possibility of having unpredictable 2 minute episodes of being frozen by pain with tears streaming from your eyes makes it difficult to do anything, including social events. Because of that, I missed my step-son’s outdoor wedding on a windy day, which was especially depressing knowing that no one there probably understood the reason why, at the last minute when the winds were gusting, I knew I couldn’t go.
Anyone who has trigeminal neuralgia understands the frustration of knowing that most people you describe the problem to, don’t believe how debilitating and unpredictable the pain episodes are, and many probably assume you’re using it as an excuse to avoid them, but maybe I’m being paranoid. If I wanted to avoid a social function, I’d use an excuse like a kidney stone that most people have heard of, rather than “supraorbital trigeminal neuralgia.”
My step-son’s father who I’ve lived with for over 30 years, saw one of my longer pain episodes when we were on our boat and the wind blew my hair a certain way. I dropped like a rock to the deck and couldn’t move or talk for 2 minutes, which seems like a very long time when you’re face is being electrocuted. Since he witnessed that, he’s never questioned the degree of severity caused by neuralgia pain.
Because I’m an emergency physician, I was trained to do supraorbital and supratrochlear nerve blocks, which I’d used in the past on patients when repairing complex facial lacerations. I started blocking those nerves in my face so that I could still function and manage the depression caused when I felt I had no control over the pain.
Each time I did the nerve blocks, the pains would stop for about two or three hours, but I had to repeat them several times in order to get throught the day treating patients. By the end of the day, my right eye would be almost swollen shut and patients would ask why my right eyebrow was bleeding. I had to stop doing television and other video interviews and I hate to think about how many patients I scared away who probably thought I’d had a stroke.
I tried the usual medications recommended for trigeminal neuralgia, like carbamazepine and gabapentin, but they did nothing but make me dizzy and groggy, so I stopped taking them. I tried all the recommended supplements, homeopathic remedies and then some, without any relief. Injecting steroids only caused a bald spot in my eyebrow.
I consulted with both a pain management doctor who specialized in nerve ablation and a surgeon who specialized in performing nerve decompression. They both laughed when I told them I was doing my own supraorbital/supratrochlear nerve blocks and said, “You must be an ER doctor”. Both of them recommended that I continue doing the nerve blocks rather than undergo nerve ablation or microvascular decompression (MVD) because the success rates and associated risks of those treatments were potentially worse than the risks of doing frequent nerve blocks.
Botox helped relax the muscles of my forehead so that I had fewer pains caused by my brows lifting when I talked, but the effective amounts needed make my brow droop and my eye look smaller on the right side.
After the first four week period of pains, they suddenly stopped, and I could finally wash and comb my hair and be in the wind without any pain, but as most people with trigeminal neuralgia experience, the pain episodes returned. For the next four years, I had cycles of between four to eight weeks of pain episodes daily, separated by one to six months of complete remission in between.
Finding a treatment that Decreased the number of pain Episodes
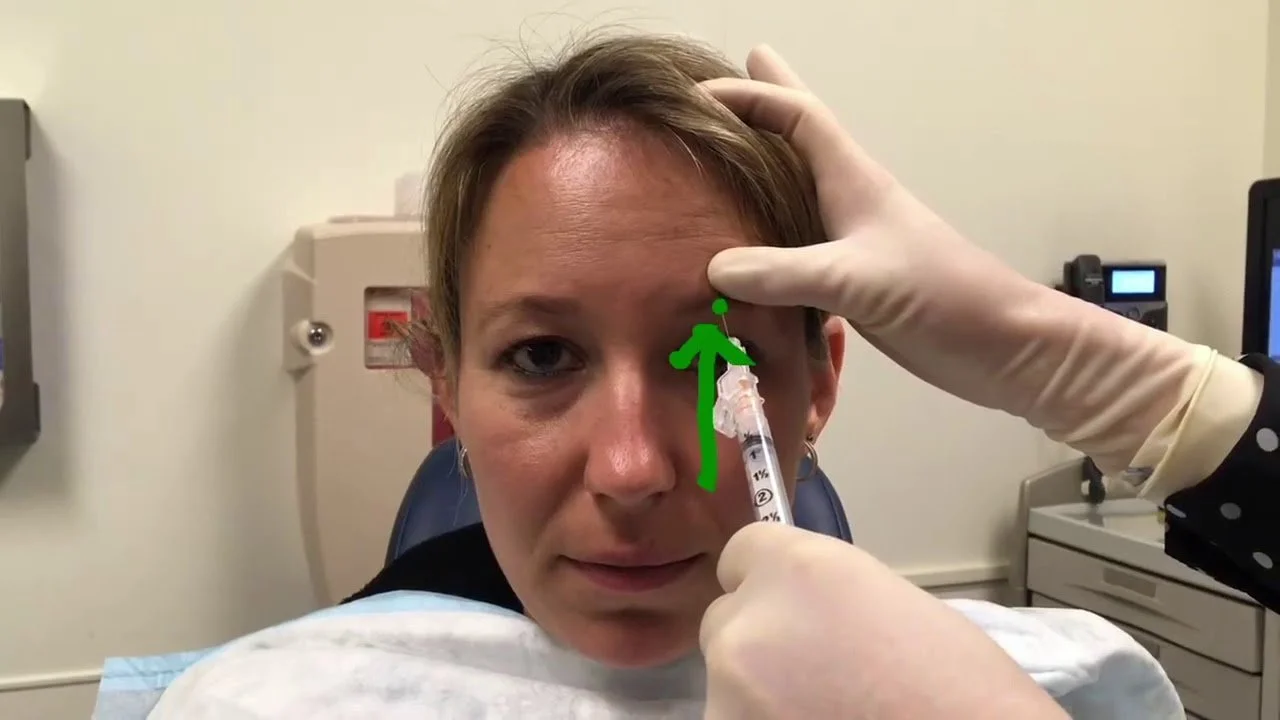
In 2024, when a new pain period started, I tried an injection mixture that new case studies had found effective with different types of nerve pain. Prolotherapy using the simple sugar, dextrose, has been used for years by mostly naturopaths to improve musculoskeletal pain. I injected the concentration of dextrose that had provided pain relief in the case studies into the area where my right supraorbital nerve exits the bone under my brow and the shock sensations immediately stopped. It was hard to believe, but for the following 48 hours, I only had a couple of bearable “zings” even when I washed my hair.
I did a second injection three days later and had no pains for the following week. When I started getting twinges of pain again, I’d repeat the injection and they’d stop again for a few days to a week. About eight weeks after the pains started, they stopped completely for a few months, and since then, I’ve done the injections when the twinges start, and I’ve never had more than a few pain episodes that lasted more than a couple of seconds.
The Evolution of My Treatments for Neuralgia
Since 2024, case studies have been published showing that Botox injection can also decrease the pain of trigeminal neuralgia, sometimes resulting in days to months of relief. My last Trigeminal Neuralgia patient had pain in her mandibular branch and I injected a large, concentrated dose of Botox and 5% dextrose where her mental nerve exited her mandible on the affected side. Five days later, her constant pain stopped for the first time in almost a year and her pain relief lasted almost 2 months, allowing her to brush her teeth normally, eat solid food, and resume working.
Keep in mind, if you’re considering using Botox for Trigeminal Neuralgia, that because it will also relax muscles overlying the nerves, you may have some asymmetric facial movements, but they will be less obvious if Botox is also used on the same muscle/s on the other side.
I’ve had excellent results using just the dextrose prolotherapy method on post herpetic neuralgia pain, which until now has been very difficult to improve. Usually only two to three treatments of injections just below the skin’s surface produce complete resolution of post herpetic pain syndrome.
Only someone who has had neuralgia pain can truly appreciate how grateful and excited I am to have found treatments that control my pain, and I smile like a maniac now every time I wash my hair or walk in the wind. I can’t imagine anything more gratifying than helping others find at least a partial solution to their neuralgia pain. Although I can’t guarantee improvement, I’m willing to provide these treatments to anyone who has neuralgia and wants to give it a try.
If you’re interested in exploring this treatment option for your neuralgia pain, request an appointment for a consultation today.
– Cynthia Elliott, MD, Skinspirations
Dr. Cindy Elliott is the owner of Skinspirations as well as the clinician training facility, ExpertEsthetics. She’s personally performed over 30,000 esthetic treatments and taught her advanced esthetic injectable and laser techniques to over 275 clinicians. That means it’s likely that if you’ve had a treatment in Tampa Bay, the provider who did it was trained by Dr. Elliott.